Country selector

United Kingdom
Country Selector: United Kingdom

Turbulent times in The Netherlands. The Slingeland Hospital in Doetinchem started in early February with a test with wireless measurement of patients’ vital sign values.
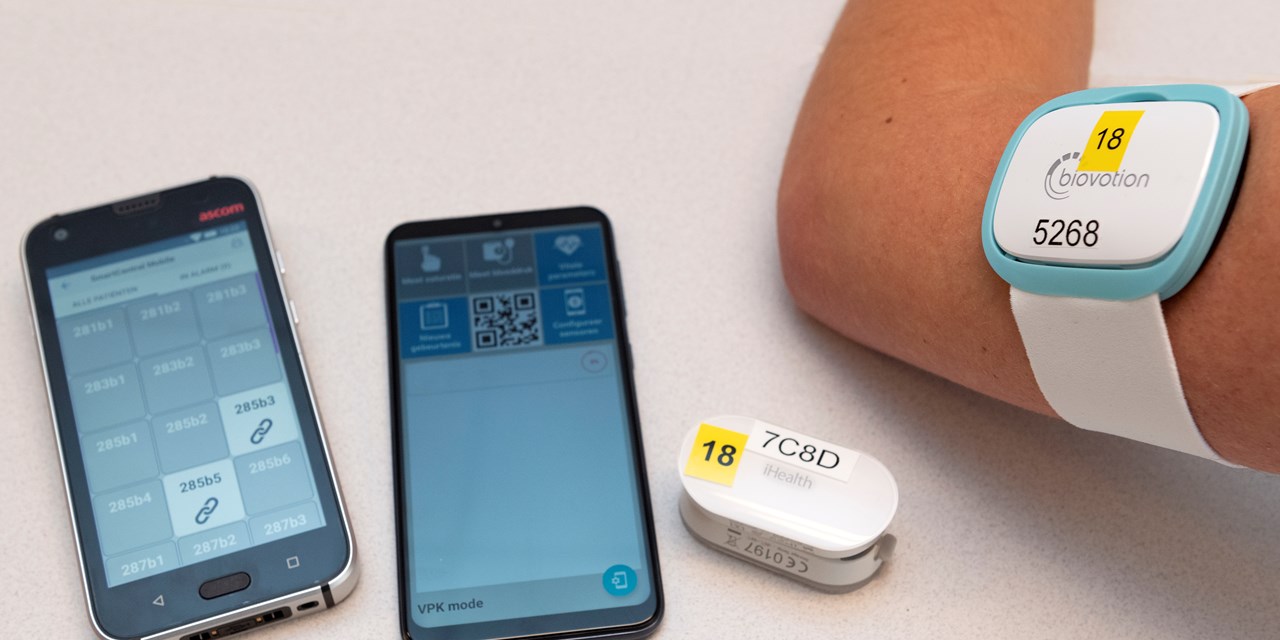
Based on these values, the risk of deterioration (Early Warning Score) or complications is calculated. After a short break to solve the latest technical challenges, the neurology and vascular surgery departments were ready to restart the trial in early March. But, just then, the COVID-19 pandemic reached the Nether-lands. This meant that all non-acute care stopped immediately, including the Sensing Clinic project with Ascom. Until the doctors asked themselves after a few days: can we use this planned continuous monitoring system for our COVID-19 patients?
In no time, the platform was set up for the COVID-19 department. This made it possible to continuously monitor COVID-19 patients who were nursed in isolation. Healthcare providers can get a non-stop view of the respiratory rate and heart rate of patients assigned to them, on their smartphone or via the dashboard in the patient file. Saturation is measured several times per hour.
These values are also monitored 24/7 from a central control room. The assigned carers are informed if the patient shows signs of deterioration. The remote measurement aim to support the healthcare professionals. Deterioration can be signaled earlier with continuous monitoring and so intervention may be possible earlier than with a point measurement.
We were, as it were, thrown in at the deep end. You have to work collaboratively when it comes to safety - that is the highest good. Do we dare to innovate? The need to change just gives the push. We fixed this together.

Malou Peppelman, Innovation program manager at the Santiz hospitals, thinks it is too early to draw firm conclusions. How much has been prevented? Does it save sleeping days? Does it benefit the quality of care? Initial case evaluations do show that there was faster insight into deterioration through the use of continuous monitoring and the assessment of the data in the control room.
We have discovered that:
If one of the sensors on the patient's body gives a notification that a value is increasing, a notification is sent to the nurse's smartphone. The data are simultaneously visible on a dashboard in the EPD and via a screen at a central monitoring location, the control room. The sensors used come from different suppliers. The Digistat Suite communication platform from Ascom is used for the central processing, enrichment and analysis of the data.
